Hundreds of special technology tour (14)] Ultimate “l(fā)ife-saving weapon” to open the door…

“This cold almost cost me my life! Thank you for giving my husband a second life ......” Outside the door of the Intensive Care Unit of the Department of Respiratory and Critical Care Medicine of the First Affiliated Hospital of Heavy Medicine, Mr. Chen's wife excitedly expressed her gratitude to the medical staff.

In mid-March this year, Mr. Chen was admitted to the intensive care unit of the Department of Respiratory and Critical Care Medicine of the First Affiliated Hospital of Heavy Medicine because of a lung infection caused by a cold that made it difficult for him to breathe.
After admission, Mr. Chen's condition continued to worsen, acute respiratory distress syndrome, severe pneumonia, both lungs image was “big white lung”. After endotracheal intubation and invasive mechanical ventilation, Mr. Chen was still unable to relieve his respiratory distress and improve his hypoxia symptoms.
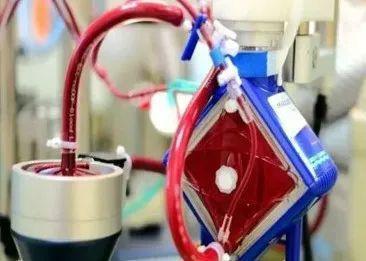
His life was hanging by a thread! After thorough evaluation and communication with the patient's family, Associate Professor Han Xiaoli and Dr. Jiang Lei from the Intensive Care Unit of the Department of Respiratory and Critical Care Medicine decided to use Extracorporeal Membrane Lung Oxygenation (ECMO) to fight for the patient's life.
The ECMO team of the Intensive Care Unit of the Department of Respiratory and Critical Care Medicine acted swiftly and successfully completed the installation of ECMO within 30 minutes from puncture and tube placement to transfer, and the patient's oxygen saturation level rose rapidly, and his heart rate, respiration, and blood pressure gradually stabilized.
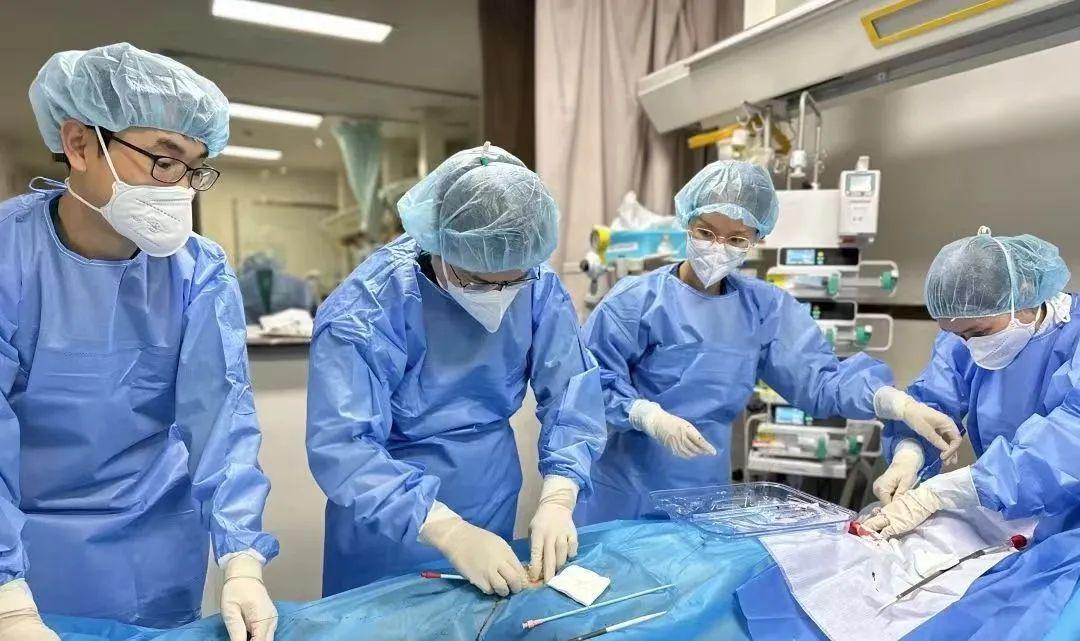
After the team's day and night care and unremitting efforts, Mr. Chen turned to safety after 8 days of ECMO treatment and was successfully withdrawn from the machine. At present, he has been successfully discharged from the hospital and recovered well.
According to Prof. Guo Shuliang, Director of Respiratory and Critical Care Medicine, Extracorporeal Membrane Lung Oxygenation (ECMO) is an advanced life support technique generally used for acute severe cardiac or respiratory failure that may be reversible and unresponsive to conventional treatments, such as severe hypoxic respiratory failure, intractable hypercapnic respiratory failure, refractory cardiogenic shock, cardiac arrest, as well as some cardiac surgeries, which is a key part of critical care It is the “ultimate weapon” in the treatment technology of intensive care unit. However, its technology is complicated and difficult to manage, and the ability to carry out ECMO technology is a reflection of a team's comprehensive treatment ability.

The ECMO team of the Department of Respiratory and Critical Care Medicine of the First Affiliated Hospital of Heavy Medicine was established in 2019, and under the leadership of Prof. Guo Shuliang, more than 20 cases of patients have been treated with ECMO, with a successful withdrawal rate of 78.9%. This year, the team has treated 5 cases of ECMO patients, including 2 cases of going outside the hospital for ECMO tube placement on the machine and transferring patients with critical respiratory failure.
The team has set up a joint management team of “medical care and technology”. In terms of medical management, the team regularly conducts multidisciplinary case discussions, and formulates optimal treatment plans for patients from the perspectives of coagulation management, hemodynamic management, volume management, nutritional support, and other dimensions.
In nursing management, the team strictly prevents hospital-acquired infections and implements single-room isolation protection for patients; develops and uses the ECMO nursing quality control checklist to implement refined nursing management for patients; closely monitors patients' condition changes 24 hours a day and reports them for timely treatment, and does a good job of handing over shifts to ensure the effective treatment and nursing safety of ECMO patients.
In terms of respiratory therapy, the team uses bedside ultrasound, chest electrical impedance imaging (EIT) and other technologies to assess patients' lung function and adjust respiratory therapy programs on a daily basis.




